Filter
97
Featured
14
3
Language
Document type
36
15
10
8
7
6
5
4
3
2
1
Countries / Regions
7
1
1
Authors & Publishers
Publication Years
Category
16
4
2
1
1
Website last accessed on 18.03.2023
Website last accessed on 18.03.2023
Buruli Ulcer Disease: Obtaining Swab Specimens for Diagnosis of M. Ulcerans Infection - Youtube video
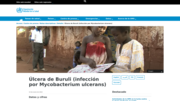
Buruli ulcer (BU) is a bacterial skin infection that is caused by Mycobacterium ulcerans and mainly affects people who reside in the rural areas of Africa and in suburban and beach resort communities in Australia.
In the 126 years since it was first described, scientists have learned a great deal about Buruli ulcer, (an ulcerating skin infection caused by the environmental bacterium, Mycobacterium ulcerans), including how to treat it. Yet, there is 1 question about this neglected tropical disease that has rem
...
Buruli ulcer (BU), a neglected tropical disease (NTD), is an infection of the skin and subcutaneous tissue caused by Mycobacterium ulcerans. The disease has been documented in many South American, Asian, and Western Pacific countries and is widespread throughout much of Africa, especially in West
...
Status of endemicity of Buruli ulcer 2023
In 2009, WHO’s Second International Conference on Buruli Ulcer Control and Research resolved to strengthen the capacity of national laboratories to confirm cases of the disease, but advised that “efforts are still needed to develop simple diagnostic tools usable in the field as well as disabilit
...
Key facts
Buruli ulcer is a chronic debilitating disease caused by an environmental Mycobacterium ulcerans.
At least 33 countries with tropical, subtropical and temperate climates have reported Buruli ulcer in Africa, South America and Western Pacific regions.
It often affects the skin an
...
Principaux faits
L’ulcère de Buruli est une infection chronique débilitante causée par la bactérie Mycobacterium ulcerans.
L’ulcère de Buruli a été signalé dans au moins 33 pays situés dans des régions au climat tropical, subtropical ou tempéré d’Afrique, d’Amérique
...
Datos y cifras
La úlcera de Buruli es una enfermedad crónica y debilitante causada por una micobacteria ambiental: Mycobacterium ulcerans.
Al menos 33 países de clima tropical, subtropical o templado han notificado casos de úlcera de Buruli en África, América del Sur y las regiones
...
The Lancet Volume 399, Issue 10327p786-797February 26, 2022
Free download after free registration
Journal of Computational Biophysics and ChemistryVol. 22, No. 01, pp. 31-41 (2023)
Countries where buruli ulcer is endemic
August 26, 2021
https://doi.org/10.1371/journal.pntd.0009678
This manual details a collaboratively developed intervention to detect and refer Buruli ulcer, Hydrocele, Leprosy
and Lymphedema cases through the use of integrated approaches at community levels. This intervention has
been developed as part of the consortium in partnership with the Nigerian Feder
...
Buruli ulcer (BU), the second most common mycobacterial disease in West Africa, is a necrotizing skin disease that can lead to high morbidity in affected patients. The disease is caused by Mycobacterium ulcerans (MU), whose major virulence factor is mycolactone. Although early infection can be treat
...
Technical Update
Areas of Africa endemic for Buruli ulcer (BU), caused by Mycobacterium ulcerans, also have a high prevalence of human immunodeficiency virus (HIV), with adult prevalence rates between 1% and 5% (Maps). However, there is limited information on the prevalence of BU–HIV coinfection.
...
A total of 18 laboratories from 13 countries participated in the four rounds of EQA: 10 laboratories from eight African endemic countries, four of which participated in all four rounds and three in three rounds. The overall results showed that the median performance of these laboratories improved ov
...
The Lancet olume 395, ISSUE 10232, P1259-1267, April 18, 2020. Buruli ulcer is a neglected tropical disease caused by Mycobacterium ulcerans infection that damages the skin and subcutis. It is most prevalent in western and central Africa and Australia. Standard antimicrobial treatment with oral rifa
...
Phillips and colleagues have shown that rifampicin combined with clarithromycin is non-inferior to RS8, and is safer. This much anticipated trial provides us with a high degree of confidence that an 8-week course of oral rifampicin and clarithromycin should now be the cornerstone of the treatment of
...