Filter
2546
Text search:
community
mobilization
Featured
227
858
Language
2469
58
38
30
21
17
13
4
4
3
2
1
1
1
1
1
1
1
1
1
1
1
Document type
1502
330
270
204
135
44
37
18
3
1
1
Countries
110
104
101
100
92
89
87
72
70
54
53
50
42
41
40
40
39
35
34
33
26
26
22
22
21
21
20
20
20
20
20
19
17
16
14
13
13
13
12
11
11
10
10
10
9
9
8
8
7
7
7
7
6
6
6
6
6
6
6
5
5
5
5
5
4
4
4
4
4
3
3
3
3
3
3
3
3
3
3
2
2
2
2
2
2
2
2
2
2
2
2
2
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
Authors & Publishers
309
120
76
67
64
63
62
58
43
31
29
26
25
17
15
15
15
14
14
13
13
13
13
13
13
12
12
12
12
11
11
10
10
10
9
9
9
9
8
8
8
8
8
8
8
8
8
7
7
7
7
7
7
7
7
7
7
7
7
7
7
7
6
6
6
6
6
6
6
6
6
6
6
6
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
Publication Years
662
1642
235
7
Category
1195
198
147
129
92
39
4
Toolboxes
170
151
131
129
94
76
72
69
61
60
56
52
49
48
48
43
32
29
28
27
24
15
10
10
3
3
1
This I-Kit provides essential information and tools for responding to an outbreak using an SBCC approach. It presents a series of nine units, each accompanied by exercise worksheets to help link the SBCC theory to practice.
The worksheets in each section are typically followed by a completed exam
...
ple. The completed examples will likely include information about an emergency that, during an actual event, might not be immediately available. This was done to illustrate the full range of information to inform a strategic communication response.
more
Situation Overview & Humanitarian Needs | July – September 2017
Towards universal access
The CBDRR Training Course is based on the CBDRR Step-by-Step Methodology and its main goal is to teach MRCS Field Staff and MRCS RCVs to use the CBDRR Manual document which acts as a support document for the implementation of CBDRR programs in Myanmar.
- In Part A, the course curriculum is pres ... ented and the participants can find a detailed schedule of their training. Furthermore, any additional information that is required by the participants such as accommodation during the training, the exact location of the training etc. will be included in Part A.
- In Part B, each of the sessions will be discussed separately. Key questions that participants should be able to answer after each session are posed and the participants are invited to note down their answer to each of the questions during or after each session to increase the learning effect.
- In Part C, the supporting training documents will be presented. more
- In Part A, the course curriculum is pres ... ented and the participants can find a detailed schedule of their training. Furthermore, any additional information that is required by the participants such as accommodation during the training, the exact location of the training etc. will be included in Part A.
- In Part B, each of the sessions will be discussed separately. Key questions that participants should be able to answer after each session are posed and the participants are invited to note down their answer to each of the questions during or after each session to increase the learning effect.
- In Part C, the supporting training documents will be presented. more
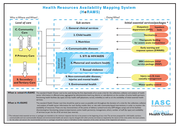
Human Resources
WHO
(2015)
excessed 27 January 2015
The funding requested in this supplementary appeal will enable UNHCR to enhance preventive, preparedness and response measures against EVD, participate in the regional and country inter-agency response and ensure continuity of operations, including preparations for the resumption of the voluntary re
...
patriation of Ivorian refugees, in the face of the Ebola crisis
more
Strategic Communication for Zika Prevention: A Framework for Local Adaptation
Alice Payne Merritt, Gabrielle Hunter, Anne Ballard et al.
ohns Hopkins Center for Communication Programs
(2017)
C1
The National Strategic Plan on Malaria Prevention and Elimination Period 2021 – 2025 seeks to build on the previous national successes of the National Institute of Malariology, Parasitology, and Entomology (NIMPE) while addressing current challenges to reduce the overall burden of malaria in the S
...
outhern and Central provinces and to initiate elimination activities in remaining focal areas of transmission throughout the country. The overall targets proposed to be reached by 2025 are:
Reduce malaria morbidity rate to below 0.015/1,000 population
Reduce malaria mortality rate to below 0.002/100,000 population
Eliminate malaria in 55 provinces
Ensure no malaria outbreaks
To address the urgent threat of drug resistance, Viet Nam has committed to accelerate efforts to eliminate locally-acquired P. falciparum by 2023.
more
Follow up to the Maseru Declaration. ZIMBABWE COUNTRY REPORT
Reporting Period: January 2013 - December 2013