Filter
4246
Text search:
disease
therapy
Featured
468
1060
Language
3941
113
103
95
38
34
33
25
11
6
5
5
5
4
4
4
3
2
2
2
2
2
2
2
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
Document type
2304
737
648
232
106
96
69
16
10
10
8
5
1
1
1
Countries
279
180
123
116
97
87
85
78
74
69
67
64
59
59
56
52
49
47
44
40
39
36
36
35
35
31
31
26
25
23
23
23
21
21
21
20
19
18
18
15
14
13
13
12
11
11
10
9
9
9
9
8
8
7
7
7
7
7
7
7
7
7
6
6
6
6
5
5
5
5
5
5
4
4
4
4
4
4
4
4
4
3
3
3
3
3
3
3
3
3
3
2
2
2
2
2
2
2
2
2
2
2
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
Authors & Publishers
565
228
165
102
81
71
65
63
62
51
41
27
26
24
23
22
21
20
20
20
19
19
18
17
17
16
15
15
15
15
15
15
14
14
14
13
13
13
13
13
13
12
12
11
11
11
11
11
11
10
10
10
10
9
9
9
9
9
8
8
8
8
8
8
8
8
8
8
8
8
7
7
7
7
7
7
7
7
6
6
6
6
6
6
6
6
6
6
6
6
6
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
5
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
4
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
3
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
2
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
Publication Years
1155
2625
444
20
2
Category
1648
490
268
190
90
71
44
2
Toolboxes
452
412
253
241
194
167
166
123
107
97
82
61
48
46
42
38
29
29
28
21
19
18
17
16
11
Clinical Practice Guidelines and Clinical Pathway for Therapy and Management of Heart Disease and Blood Vessels in Indonesia
The document provides comprehensive guidelines on cholera outbreak management, including prevention, diagnosis, and treatment. It emphasizes rapid response measures, the importance of rehydration therapy (oral and intravenous), and public health int
...
erventions such as water sanitation, hygiene promotion, and disease surveillance to control the spread of cholera in affected communities. It is designed as a resource for healthcare providers and public health officials.
more
The document outlines comprehensive guidelines for managing cholera outbreaks in South Africa, focusing on prevention, diagnosis, treatment, and public health measures. It emphasizes the importance of rehydration therapy, sanitation, clean water acc
...
ess, and community involvement to control the spread of the disease. It also provides protocols for handling outbreaks, including case identification, laboratory confirmation, and multi-sectoral coordination to reduce morbidity and mortality rates.
more
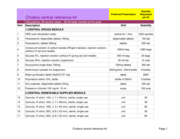
The document lists the components of various cholera kits designed for managing cholera outbreaks. It includes items for rehydration therapy (e.g., oral rehydration salts and IV fluids), medications, sanitation supplies, diagnostic tools, and logist
...
ical materials such as cholera beds and water purification systems. These kits aim to support healthcare providers in treating patients, preventing the spread of the disease, and maintaining hygiene in affected areas.
more
1.HIV infections – drug therapy. 2.Anti-HIV agents – adverse effects. 3.Anti-retroviral agents. 4.Benzoxazines – adverse effects. 5.Pregnancy. 6.Disease transmission, Vertical - prevention and
...
control. 7.Treatment outcome. I.World Health Organization
more
Heart failure with a reduced ejection fraction (HFrEF) is a condition frequently encountered by healthcare professionals and, in order to achieve the best outcomes for patients, needs to be managed optimally. This guideline document is based on the European Society of Cardiology Guidelines for the t
...
reatment of acute and chronic heart failure published in 2016, and summarises what is considered the best current management of patients with the condition. It provides information on the definition, diagnosis and epidemiology of HFrEF in the African context. The best evidence-based treatments for HFrEF are discussed, including established therapies (beta-blockers, ACE-i/ARBs, mineralocorticoid receptor antagonists (MRAs), diuretics) that form the cornerstone of heart failure management as well as therapies that have only recently entered clinical use (angiotensin receptor-neprilysin inhibitor (ARNI), sodium/glucose cotransporter-2 (SGLT2) inhibitors). Guidance is offered in terms of more invasive therapies (revascularisation, implantable cardioverter defibrillators (ICDs) and cardiac resynchronisation therapy (CRT) by implantation of a biventricular pacemaker with (CRT-D) or without (CRT-P) an ICD, left ventricular assist device (LVAD) use and heart transplantation) in order to ensure efficient use of these expensive treatment modalities in a resourcelimited environment. Furthermore, additional therapies (digoxin, hydralazine and nitrates, ivabradine, iron supplementation) are discussed and advice is provided on general preventive strategies (vaccinations). Sections to discuss conditions that are particularly prevalent in sub-Saharan Africa (HIV-associated cardiomyopathy (CMO), peripartum CMO, rheumatic heart disease, atrial fibrillation) have been added to further improve clinical care for these commonly encountered disease processes.
more
Hepatitis B (HBV) infection is a major public health problem and cause of chronic liver disease.
The 2024 HBV guidelines provide updated evidence-informed recommendations on key priority topics. These include expanded and simplified treatment cri
...
teria for adults but now also for adolescents; expanded eligibility for antiviral prophylaxis for pregnant women to prevent mother-to-child transmission of HBV; improving HBV diagnostics through use of point-of-care HBV DNA viral load and reflex approaches to HBV DNA testing; who to test and how to test for HDV infection; and approaches to promote delivery of high-quality HBV services, including strategies to promote adherence to long-term antiviral therapy and retention in care.
The 2024 guidelines include 11 updated chapters with new recommendations and also update existing chapters without new recommendations, such as those on treatment monitoring and surveillance for liver cancer.
more
The document provides comprehensive guidance for people with COPD, covering treatment and medication management, oxygen therapy, mucus control, exercise, smoking cessation, nutrition, associated conditions, and strategies to prevent exacerbations. I
...
t emphasizes patient education, self-management, and working closely with healthcare providers to enhance well-being and control of the disease.
more
The document provides practical guidance for individuals with COPD, covering topics such as medication management, oxygen therapy, mucus control, physical exercise, smoking cessation, nutrition, associated conditions, and how to prevent and manage e
...
xacerbations. It emphasizes the importance of patient education, adherence to treatment plans, and collaboration with healthcare providers to improve quality of life and disease outcomes.
more
Preventing tuberculosis infection from progressing to tuberculosis disease is a crucial component of the goal to eliminate tuberculosis. When deciding on the use of tuberculosis preventive therapy a
...
mong household contacts, policy makers regularly ask questions, such as whether tuberculosis preventive therapy is effective, safe, and feasible in a programme setting and what it will cost. For contact management and tuberculosis preventive therapy for multidrug-resistant and rifampicin-resistant tuberculosis, studies from high-income and low-income countries have shown feasibility, safety, and effectiveness.
However, there is scarce information on the cost of tuberculosis preventive therapy for multidrug-resistant and rifampicin-resistant tuberculosis. In The Lancet Global Health, Peter Dodd and colleagues show that household contact management strategies are cost-effective even in low-income and middle-income countries, which has important policy implications for achieving the END TB Strategy goals.
more
The cardiovascular disease continuum begins with risk factors such as diabetes mellitus (DM), progresses to vasculopathy and myocardial dysfunction, and finally ends with cardiovascular death. Diabetes is associated with a 2- to 4-fold increased ris
...
k for heart failure (HF). Moreover, HF patients with DM have a worse prognosis than those without DM. Diabetes can cause myocardial ischemia via micro- and macrovasculopathy and can directly exert deleterious effects on the myocardium. Hyperglycemia, hyperinsulinemia, and insulin resistance can cause alterations in vascular homeostasis. Then, reduced nitric oxide and increased reactive oxygen species levels favor inflammation leading to atherothrombotic progression and myocardial dysfunction. The classification, diagnosis, and treatment of HF for a patient with and without DM remain the same. Until now, drugs targeting neurohumoral and metabolic pathways improved mortality and morbidity in HF with reduced ejection fraction (HFrEF). Therefore, all HFrEF patients should receive guideline-directed medical therapy. By contrast, drugs modulating neurohumoral activity did not improve survival in HF with preserved ejection fraction (HFpEF) patients. Trials investigating whether sodium-glucose cotransporter-2 inhibitors are effective in HFpEF are on-going. This review will summarize the epidemiology, pathophysiology, and treatment of HF in diabetes.
more
The video titled "Personalizing Selection of Inhaled Delivery Systems in COPD" discusses the complexities healthcare professionals face when prescribing inhaled therapies for chronic obstructive pulmonary disease (COPD). It highlights the diverse ra
...
nge of available medications and delivery systems, noting that while medication categorization has been extensively studied, guidance on selecting appropriate inhaler devices remains limited and lacks consensus in COPD guidelines. The video proposes a novel strategy to address this issue, aiming to enhance the personalization of inhaled therapy for COPD patients.
more
Leprosy will be eliminated when we detect all patients and cure them by using multidrug therapy (MDT).
Elimination means bringing the disease burden down to a very low level. This will lead to a
...
reduction in the source of infection, so that leprosy is likely to disappear naturally as it already has in many parts of the world. WHO has defined “elimination” as a prevalence rate of less than 1 case per 10,000 inhabitants.
more
Over 90% of the morbidity and mortality related to chronic obstructive pulmonary disease (COPD) and asthma occurs in low-income and middle-income countries (LMICs) due to well documented factors including decreased access to screening, trained healt
...
h professionals, and therapies for disease management. Inhaler therapy (eg, aerosolised medications by inhalation, nebulisation, or propellant) is the mainstay of treatment for COPD and asthma. Adherence to maintenance medications for COPD and asthma results in improved lung function and quality of life, as well as decreased hospitalisation and mortality. WHO have included short-acting beta-agonists, long-acting muscarinic antagonists, and inhaled corticosteroids on the essential medications list, with a target goal of achieving 80% availability of these medications in public and private facilities. However, despite these efforts, accessibility, and affordability of medications for COPD and asthma remains scarce.
more
Buruli ulcer caused by Mycobacterium ulcerans is a neglected tropical disease characterized by extensive ulceration involving predominantly the upper and lower limbs of patients. The disease is comm
...
on in rural tropical communities in West and Central Africa, where access to proper health care is limited. Pathogenesis of the characteristic painless ulcers is linked to the elaboration by M. ulcerans of a lipid toxin called mycolactone that has potent cytopathic, immunosuppressive, and analgesic effects on a host of cells in cutaneous tissues. Mycolactone is known to profoundly inhibit secretion of a plethora of proteins that are essential for wound healing. Even though a combination antibacterial therapy of streptomycin and rifampicin for 8 weeks is effective for treatment, it relies on good and appropriate wound management to prevent secondary bacterial infections and improve healing. Evidence-based interventions for wound care in Buruli ulcer disease are often lacking and have relied on expert advice and recommendations. Surgical interventions are limited to debridement of necrotic tissue and grafting of extensive ulcers, usually after antibiotic therapy. Patients’ rehabilitation is an important component of care to reduce disabilities associated with the disease and proper integration into the community after treatment.
more
The Cholera Q&A Fact Sheet provides essential information about cholera, including its causes, symptoms, treatment, and prevention. Cholera is an acute diarrheal disease caused by Vibrio cholerae, which spreads through contaminated water and food. I
...
t leads to rapid dehydration and can be fatal if untreated. Symptoms range from mild diarrhea to severe dehydration, shock, and death.
Treatment primarily involves Oral Rehydration Therapy (ORT) to replace lost fluids, and in severe cases, intravenous fluids. Antibiotics are generally not recommended for mass treatment. Prevention focuses on safe drinking water, sanitation, hand hygiene, and proper food handling.
The document also discusses cholera vaccination, with three WHO-approved oral vaccines available. However, vaccines should be used alongside other control measures. The Global Task Force on Cholera Control (GTFCC) aims to eliminate cholera transmission in 20 countries by 2030 through improved sanitation, vaccination, and rapid outbreak response.
more
Heart failure (HF) is a leading global public health problem with >64 million prevalent cases globally. Patients with HF with reduced ejection fraction (HFrEF) from low- and middle-income countries experience a 22% to 58% higher 1-year mortality rate than those in high-income countries.1 Guideline-d
...
irected medical therapy (GDMT) consisting of ACE (angiotensin-converting enzyme) inhibitors or ARB (angiotensin receptor blockers) or ARNI (angiotensin receptor-neprilysin inhibitors), β-blockers, MRA (mineralocorticoid receptor antagonists), and SGLT2 (sodium-glucose cotransporter 2) inhibitors substantially reduces mortality among patients with HFrEF. These medicines are among the most cost-effective interventions and are thus included as the highest priority health system interventions recommended by the Disease Control Priorities Project.2 Despite this high-quality evidence, GDMT remains widely underutilized in low- and middle-income countries resulting in widespread undertreatment of patients with HFrEF due to health system-, provider-, and patient-level barriers.1 National essential medicines lists (EMLs) promoted by the World Health Organization (WHO) guide countries on which medications to purchase in the setting of limited resources and have resulted in higher procurement and availability of essential medicines in the public sector.3 We provide a cross-sectional analysis of national EMLs in 53 low- and middle-income countries, and availability, price, and affordability of GDMT in select countries to identify potential barriers to access to these essential medicines for patients with HFrEF.
more
The pamphlet "What is Addiction" explains addiction as a chronic, relapsing brain disease characterized by compulsive drug seeking and use, despite harmful consequences. It highlights the dangers of different drug categories, including sedatives, st
...
imulants, and hallucinogens, and their potential health and behavioral impacts. The document emphasizes the importance of combined medication and behavioral therapy in the treatment process, including detoxification, ongoing therapy, and relapse prevention. Additionally, it provides contact information for addiction treatment resources.
more
The document provides comprehensive guidelines on cholera outbreak management, including prevention, diagnosis, and treatment. It emphasizes rapid response measures, the importance of rehydration therapy (oral and intravenous), and public health int
...
erventions such as water sanitation, hygiene promotion, and disease surveillance to control the spread of cholera in affected communities. It is designed as a resource for healthcare providers and public health officials.
more
Belgian Antibiotic Policy Coordination Committee Policy paper for the 2014-2019 term
Erica Balligand, Michiel Costers and Evelyne Van Gastel
Belgian Antibiotic Policy Coordination Committee
(2014)
C2
Antimicrobial resistance represents a big threat to public health. The Centers for Disease Control and Prevention (CDC) estimate that every year two million Americans are infected with a (multi-)drug resistant bacterium, resulting in 23,000 deaths.
...
The WHO has repeatedly drawn attention to this major health issue. In the worst-case scenario, we will shortly run out of effective antibiotics. Surgery and cancer therapy will then become very dangerous due to the risk of infection associated with such treatments. (Organ) transplantation will become close to impossible as the immunosuppression necessary for transplant patients makes them highly vulnerable to infections. Some infections we can easily treat today could turn deadly. It is therefore conceivable that infectious diseases once again become the leading cause of death as in early 20th century.
more