Filter
724
Text search:
oxygen
therapy
Featured
144
137
Language
Document type
305
216
70
63
18
14
13
12
4
3
2
2
2
Countries
71
29
23
22
16
14
14
13
13
13
12
11
10
10
8
8
7
7
6
6
6
6
6
6
5
4
3
3
3
3
3
3
3
3
3
2
2
2
2
2
2
2
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
Authors & Publishers
Publication Years
Category
307
112
76
34
19
12
9
Toolboxes
146
53
34
27
25
22
21
17
15
15
10
9
9
8
8
7
6
5
4
3
3
2
2
2
This manual focuses on the availability and clinical use of oxygen therapy in children in health facilities by providing the practical aspects for health workers, biomedical engineers, and administr
...
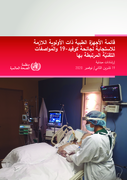
This collection of posters are intended for health care workers, biomedical engineers and staff of health facilities in charge of caring, cleaning, decontaminating and sterilizing respiratory medical equipment in hospitals and health facilities. They include checklists to ensure the optimal infectio
...
4 April 2020
This interim guidance on oxygen sources and distribution strategies for COVID-19 treatment has been adapted from WHO and UNICEF’s technical specifications and guidance for oxygen
...
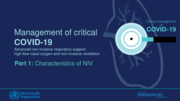
WHO recommends prompt recognition of progressive acute hypoxaemic respiratory failure when a patient with respiratory distress is failing to respond to standard oxygen therapy and adequate preparati
...
Management of critical COVID-19: Acute hypoxaemic respiratory failure and COVID-19: Recognize ARDS
recommended
WHO recommends prompt recognition of progressive acute hypoxaemic respiratory failure when a patient with respiratory distress is failing to respond to standard oxygen therapy and adequate preparati
...
Priority medical devices list for the COVID-19 response and associated technical specifications
recommended
23 February 2021
This document describes the medical devices required for the clinical management of COVID-19, selected and prioritized according to the latest available evidence and interim guidelines. This includes: oxygen
...
23 February 2021
This document describes the medical devices required for the clinical management of COVID-19, selected and prioritized according to the latest available evidence and interim guidelines. This includes: oxygen
...
23 February 2021
This document describes the medical devices required for the clinical management of COVID-19, selected and prioritized according to the latest available evidence and interim guidelines. This includes: oxygen
...
The document provides comprehensive guidance for people with COPD, covering treatment and medication management, oxygen therapy, mucus control, exercise, smoking cessation, nutrition, associated con
...
The document provides practical guidance for individuals with COPD, covering topics such as medication management, oxygen therapy, mucus control, physical exercise, smoking cessation, nutrition, ass
...
If you have COVID-19 and are caring for someone or yourself at home, what is the treatment protocol? What is WHO’s guidance on Remdesivir and convalescent plasma therapy? How to monitor oxygen at
...
9 April 2020
WHO has published the guidance “Clinical management of severe acute respiratory infection (SARI) when COVID-19 disease is suspected” This document is intended for clinicians taking care of hospitalized adult and paediatric patients with severe acute respiratory infection (SARI) whe
...
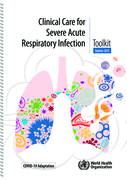
First published in 2020, this toolkit is intended for clinicians working in acute care, managing adult and paediatric patients with acute respiratory infection, including severe pneumonia, acute respiratory distress syndrome, sepsis and septic shock. The main objective is to provide key tools for us
...
Covid-19 Test to Treat Guidelines
recommended
n response to the outbreak, the Africa Centres for Disease Control and Prevention (Africa CDC) has been supporting African Union Member States in responding to the COVID-19 pandemic through a variety of interventions such as non-pharmaceutical interventions, quarantine, testing, isolation, contact t
...
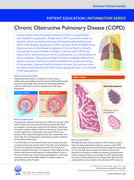
The document by the American Thoracic Society provides an overview of Chronic Obstructive Pulmonary Disease (COPD), explaining its causes, such as smoking and environmental factors, symptoms like breathlessness and chronic cough, and diagnostic methods including spirometry. It discusses treatment st
...
The cardiovascular disease continuum begins with risk factors such as diabetes mellitus (DM), progresses to vasculopathy and myocardial dysfunction, and finally ends with cardiovascular death. Diabetes is associated with a 2- to 4-fold increased risk for heart failure (HF). Moreover, HF patients wit
...
BMJ Global Health2020;5:e002786. doi:10.1136/bmjgh-2020-002786
This poster is intended for health workers and other personnel on the safety and mitigation measures that need to be adhered to when dealing with medical oxygen. Medical oxygen, either in liquid or
...