Filter
8304
Filtered Results: 8304
Text search:
transmissao
Featured
Recommendations
787
New Publications
2141
Language
Document type
No document type
4304
Guidelines
1305
Studies & Reports
1213
Manuals
394
Strategic & Response Plan
355
Fact sheets
313
Training Material
133
Situation Updates
86
Infographics
62
Resource Platforms
46
Videos
37
Online Courses
34
Brochures
18
Dashboards/Maps
3
App
1
Countries / Regions
Global
296
India
279
Congo, Democratic Republic of
223
Sierra Leone
204
Kenya
192
Liberia
191
Senegal
171
Nigeria
160
Ethiopia
138
Western and Central Europe
132
Africa
130
Tanzania
130
Rwanda
128
South Africa
128
Uganda
125
Latin America and the Carribbean
123
Guinea
122
Burkina Faso
113
Malawi
112
Zambia
111
Nepal
104
West and Central Africa
88
Brazil
88
Bangladesh
85
Haiti
75
Ghana
71
Myanmar / Burma
71
Mozambique
69
Namibia
66
Mali
64
Russia
63
Zimbabwe
62
Benin
61
East and Southern Africa
60
Syria
59
Middle East and North Africa
58
Philippines
56
Ukraine
54
Cameroon
54
Côte d’Ivoire / Ivory Coast
53
Eastern Europe
52
Madagascar
52
Lesotho
49
Cambodia
47
Germany
47
South–East Asia Region
45
Yemen
45
Colombia
44
South Sudan
43
Asia
42
Niger
35
Indonesia
35
Venezuela
33
Central African Republic
33
Botswana
33
Eastern Europe and Central Asia
26
Pakistan
26
Argentina
25
Angola
25
Chad
24
Eswatini/ Swaziland
23
Paraguay
22
Guinea-Bissau
19
Somalia
19
Togo
18
Afghanistan
18
Western Pacific Region
18
Peru
15
Vietnam
15
Thailand
14
Sudan
14
Tajikistan
13
Chile
13
Burundi
13
Spain
13
Ecuador
13
Albania
12
Bolivia
11
Iraq
11
China
10
France
10
Lebanon
10
Sri Lanka
9
Georgia
9
El Salvador
8
Jordan
8
Saudi Arabia
8
Timor Leste/ East Timor
7
North America
7
Papua New Guinea
7
Moldova
7
Laos
6
Congo-Brazzaville
6
Malaysia
6
Morocco
6
Italy
6
USA
6
Dominican Republic
6
Southern Africa
6
Djibouti
6
Egypt
6
Honduras
6
North Macedonia
5
Gambia
5
Armenia
5
Luxembourg
5
Tunisia
5
Palestine
5
Mexico
4
Turkey
4
Iran
4
Canada
4
United Kingdom
4
Portugal
4
Libya
4
Uzbekistan
3
Qatar
3
Mauritania
3
Turkmenistan
3
Belgium
3
Algeria
3
Nicaragua
3
Cuba
3
Guatemala
3
North Korea
2
Australia
2
Kazakhstan
2
Singapore
2
Estonia
2
Ireland
2
Uruguay
2
Japan
2
Belarus
2
Bhutan
2
Switzerland
1
Serbia
1
Fiji
1
Austria
1
Mongolia
1
Cape Verde
1
Denmark
1
Maldives
1
Mauritius
1
South Korea
1
Morocco
1
Israel
1
Latvia
1
Belize
1
Costa Rica
1
Guyana
1
Panama
1
Romania
1
Greece
1
Poland
1
Solomon Islands
1
Authors & Publishers
Publication Years
Category
Countries
3257
Clinical Guidelines
580
Key Resources
351
Women & Child Health
292
Public Health
264
Capacity Building
148
Pharmacy & Technologies
74
Annual Report MEDBOX
1
Toolboxes
COVID-19
1260
HIV
849
TB
517
Ebola & Marburg
514
NTDs
447
Rapid Response
235
Malaria
211
AMR
208
Planetary Health
187
Zika
177
Mental Health
155
Caregiver
145
Cholera
127
Refugee
96
Conflict
95
2.0 Rapid Response
94
Polio
79
Natural Hazards
76
Pharmacy
74
Global Health Education
71
Disability
50
Health Financing Toolbox
50
NCDs
26
Specific Hazards
23
Social Ethics
11
Typhoon
2
South Sudan
1
The Zambia Population Based HIV impact assessment of 2016, reported the prevalence of viral hepatitis in Zambia as ranging between 5.6% among adults aged 15 to 59% in the general population, and 7.1% among HIV infected individuals. It is estimated that the majority of persons with chronic hepatitis ...
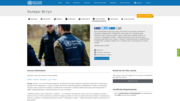
Since the re-emergence of monkeypox in Nigeria in September 2017, the Nigeria Centre
for Disease Control(NCDC) has continued to receive reports and respond to cases of the
disease from States across the country. Between September 2017 when the outbreak started and November 2018, about 300 suspecte...
Холера: Вступ
recommended
Цей ознайомлювальний курс надає загальний огляд холери, включаючи принципи профілактики та боротьби з нею. Крім того, учасники курсу дізнаються про Глобальну робо...
Buruli ulcer is a disease caused by the environmental pathogen Mycobacterium ulcerans that affects skin and soft tissue. It was first described in Australia in 1948 and has been reported in several sub-Saharan African countries since the late 19th century. The disease mainly affects children in rura...
The technical note by the Global Task Force on Cholera Control (GTFCC) discusses the use of Oral Cholera Vaccines (OCVs) for international workers and travelers in cholera-affected areas. It reviews the effectiveness of WHO-prequalified vaccines (Dukoral®, Shanchol™, and Euvichol®), emphasizing ...
This document is intended for use by state and local health departments and healthcare facilities and serves as general guidance for the initial response for the containment of novel or targeted multidrug-resistant organisms (MDROs) or resistance mechanisms. It is not intended to describe all the ac...
In the 126 years since it was first described, scientists have learned a great deal about Buruli ulcer, (an ulcerating skin infection caused by the environmental bacterium, Mycobacterium ulcerans), including how to treat it. Yet, there is 1 question about this neglected tropical disease that has rem...
This is a case-ascertained prospective investigation of all identified health care contacts working in a health care facility in which a laboratory confirmed 2019-nCoV infected patient (see 2.2 Study population) receives care. Note that this study can be done in health care facilities at all 3 level...
Cette note d'orientation élaborée par l'UNICEF explique comment le secteur WASH peut mettre en œuvre des mesures de prévention et de contrôle des infections dans les ménages et les communautés. Elle met l'accent sur la réduction de l'exposition à la maladie dans les milieux communautaires e...
Although Buruli ulcer, tuberculosis, and leprosy are the three most common mycobacterial diseases, One Health dimensions of these infections remain poorly understood. This narrative review aims at exploring the scientific literature with respect to the presence of animal reservoir(s) and other envir...
Buruli ulcer (BU), the second most common mycobacterial disease in West Africa, is a necrotizing skin disease that can lead to high morbidity in affected patients. The disease is caused by Mycobacterium ulcerans (MU), whose major virulence factor is mycolactone. Although early infection can be treat...
According to WHO, infection prevention and control (IPC) is a scientific approach and practical solution designed to prevent harm caused by infection to patients and health workers. It is grounded in infectious diseases, epidemiology, social science and health system strengthening. IPC occupies a un...
Le Plan Stratégique Multisectoriel d’Élimination du Choléra en République Démocratique du Congo (2013-2017) vise à réduire l’incidence du choléra à moins d’un cas pour 100 000 habitants. Ce plan repose sur une approche multisectorielle, combinant santé, eau, hygiène et assainissemen...
This document proposes surveillance objectives and describes global standards for a minimal basic respiratory disease surveillance system for the monitoring of influenza. The agreement on objectives allows for the prioritization of the many facets of influenza that might be measured and tracked. Use...
Planning for public health emergencies should ensure that capabilities developed during previous emergencies are maintained, incorporated, and put into practice when a new event of public health concern arises. Investments in pandemic preparedness lead to more rapid detection and a stronger response...
The conditionality of this recommendation is largely driven by the current higher unit cost of pyrethroid-PBO ITNs compared
to pyrethroid-only LLINs and therefore the uncertainty of their cost-effectiveness. Furthermore, as PBO is less wash-resistant
than pyrethroids, its bioavailability declines ...
The revised guidelines contain recommendations for specific administrative, environmental controls and respiratory protection, following the assessment made by an external group of experts convened as members of the Guideline Development Group. Moreover, these guidelines focus on interventions speci...
La résistance aux antimicrobiens Esurvient lorsque les micro-organismes (bactéries, champignons, virus et parasites) évoluent quand ils sont exposés à des médicaments antimicrobiens (comme les antibiotiques, les antifongiques, les antiviraux, les antipaludiques et les anthelminthiques).
On ap...
Ce cours fournit des informations sur ce que les établissements devraient faire afin d'être prêts à réagir face à un cas de virus respiratoire émergent tel que le nouveau coronavirus, sur la manière d'identifier un cas lorsqu'il se présente, et sur la façon correcte de mettre en place des ...